One-third (33.1 percent) of people age 45 and older who are of healthy weight—defined by BMI in the 18.5 to 24.99 range—now have prediabetes, says Arch Mainous, PhD, researcher and department chair of Health Services Research, Management and Policy at the University of Florida. According to the study, this percentage increased from 22 percent in 1994, and it accounts for about 6 million to 7 million people.
What’s the reason for this trend of diabetes in normal weight people? Well, it’s complicated, but Mainous first points to people’s overall reduction in physical activity and an increasingly common body composition that trends toward softening: less lean muscle tissue and more fatty tissue. In healthy weight people with prediabetes and type 2 diabetes, sedentary lifestyle, activity level and sitting time distinguishes them, he says. Mainous’ research shows this group has lower grip strength than its no-diabetes counterparts, grip strength bein g a proxy for lean muscle mass. “While losing muscle mass as we age is a natural process, it is accelerated by inactivity,” he says.
g a proxy for lean muscle mass. “While losing muscle mass as we age is a natural process, it is accelerated by inactivity,” he says.
Other factors contributing to a growing number of healthy weight individuals with elevated blood sugar? One culprit could be limitations with the BMI test. BMI is a measure of body mass index based on a basic equation of a person’s height and weight, but doesn’t take muscle mass, fat tissue, age or other factors into account. Some experts believe BMI is not a good measurement of how metabolically healthy a person is.
“BMI doesn’t measure the fat tissue we carry,” says Joel Zonszein, M.D., professor of clinical medicine (endocrinology) at Albert Einstein College of Medicine in New York. “You can be thin and still have too much fat tissue, especially around the middle of the body where it has metabolic effects,” he says.
“Other factors for the trend,” says Zonszein, “include eating too many processed foods, exposure to chemicals and pollutants, and even the health of the microbiome,” the trillions of gut bacteria which were once believed to be isolated in the gut but which we now know communicate with the rest of the body and can influence the development of diseases.
Here are five things you can do to battle this growing trend:
1. Get tested for diabetes. Mainous is involved in a push to update testing recommendations for all adults 40 and up. The U.S. Preventative Task Force currently recommends diabetes testing only for people 40 to 70 who are overweight or obese. This isn’t without controversy—some in the medical community believe that labeling large amounts of people with prediabetes “overmedicalizes” them and creates more of a problem. Ask your healthcare provider if a diabetes test is a good idea for you.
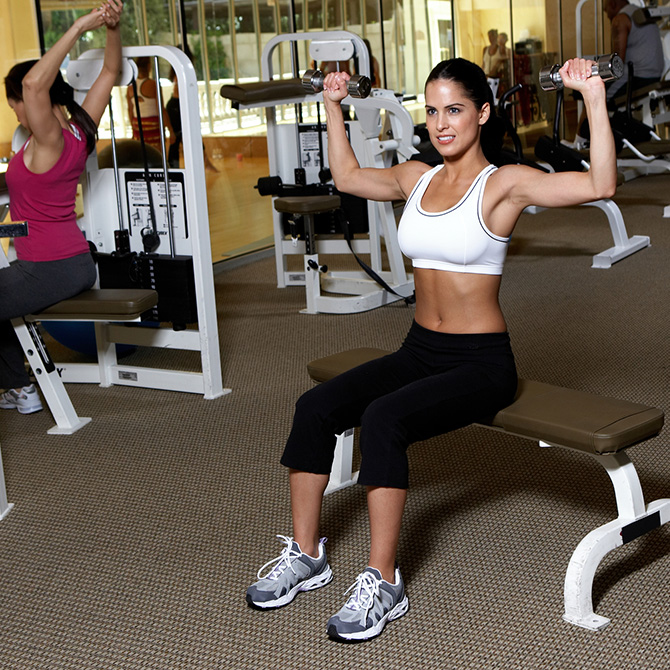
2. Keep your lean muscle mass up. This means get moving, but not just with cardio. Experts agree the best way to build muscle is with strength and resistance training, which improves the muscles’ response to insulin. Aim for two days a week of resistance training and couple with three to four days a week of at least 30 minutes each of cardiovascular exercise, says Yehuda Handelsman, M.D., medical director of the Metabolic Institute of America.
3. Don’t focus on the scale. People say they weigh the same as they did in college but that may not be the right answer, says Mainous. Instead of measuring changes in your body based on the scale alone, look at yourself in the mirror. If you think your body looks a little too soft, it probably is. Remember in some cases, gaining weight may be OK, says Mainous, if you are increasing lean muscle mass at the same time.
4. Eat well. Experts agree that a healthful, balanced diet is paramount to diabetes prevention. A 2014 study in the Journal of Education  and Health Promotion reports that a diet rich in vegetables, fruits, legumes, nuts and fish can help prevent diabetes. Aim for no more than 45 percent of your daily calorie intake from complex carbohydrate sources (green vegetables, whole grains, beans, lentils, sweet potatoes, corn and peas, for example) and the remainder from with lean proteins and healthy oils, says Handelsman. Do avoid refined carbohydrates and reduce saturated fats.
and Health Promotion reports that a diet rich in vegetables, fruits, legumes, nuts and fish can help prevent diabetes. Aim for no more than 45 percent of your daily calorie intake from complex carbohydrate sources (green vegetables, whole grains, beans, lentils, sweet potatoes, corn and peas, for example) and the remainder from with lean proteins and healthy oils, says Handelsman. Do avoid refined carbohydrates and reduce saturated fats.
5. Stay on track. It’s oh so easy—and the research shows the same—to not take the steps you need to control your blood sugar. It’s called being a human being, says Handelsman. Outline your plan and really stick with it. If you get off course with movement or eating, don’t stay there for long.
Subscribe to Delicious Living's e-newsletter for weekly news and recipes
Check out our collection of free cookbooks and eGuides